Thank you to Dr. Allen for letting us share this video.
Let’s see more of what rare eye diseases that you can have below!
Are you curious about the most astonishing and rare eye diseases in humans that can affect You?
From a mysterious condition that causes your eyes to turn blue, to an autoimmune disorder that can cause blindness, there are some truly astonishing and remarkable rare eye diseases out there. Learn about the causes, symptoms, and treatments for these rare eye diseases in humans so you can be aware of them and take preventative measures if necessary.
Early detection is key when it comes to getting the proper treatment for any of these conditions. So don’t wait until it’s too late – read this article now and learn all about seven amazing yet dangerous rare eye diseases in humans!
Keep reading to find out more about these fascinating yet serious medical conditions!
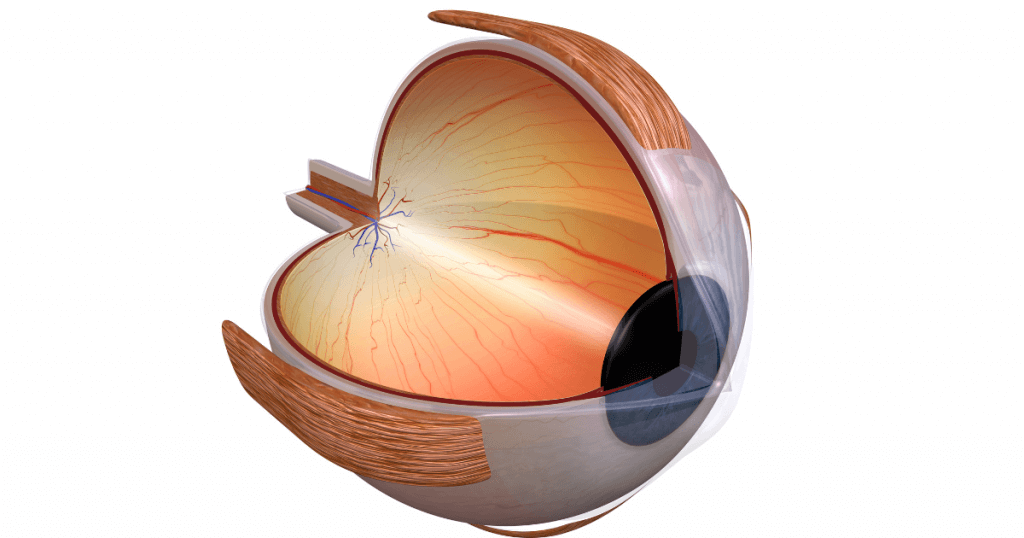
Rare eye diseases in humans can be perplexing and mysterious, but they are also very serious medical conditions that can cause significant vision problems or even total blindness. From autoimmune diseases to genetic syndromes, these rare eye diseases in humans can affect the eyes, including the cornea, sclera, iris, and retina.
The causes and symptoms of these conditions can vary greatly depending on the particular rare eye disease.
The following are eleven astonishing list of rare eye diseases that you should be aware of:
Heterochromia Iridis – The Mysterious Condition That Causes Your Eyes to Turn Blue

Heterochromia Iridis is a rare eye condition resulting in the discoloration of one or both of the eyes. This fascinating phenomenon has been seen in humans and other animals, particularly cats and dogs. It can be present at birth or acquired later in life due to illness or injury. In some cases, it is associated with genetic disorders, such as Waardenburg Syndrome or Sturge-Weber Syndrome.
Heterochromia Iridis occurs when the iris of one eye is differently colored from the other. The most common form of Heterochromia Iridis causes both eyes to be different in color. This is called “complete heterochromia.” Other forms of the condition cause one eye to have different colored regions (called “sectoral heterochromia”) or one eye to be a mixture of two colors (called “central heterochromia”). In some cases, one eye may even turn blue.
In humans, Heterochromia Iridis is relatively rare. It is estimated to affect less than 200,000 people worldwide. Although the exact cause of Heterochromia Iridis is not known, it is believed to be linked to genetic factors or a disruption in melanin production. Melanin is responsible for producing eye color and can be disrupted by disease, medication, or injury.
There is no treatment for Heterochromia Iridis and it does not pose any health risks. However, depending on the type of Heterochromia Iridis, vision may be affected in certain cases. People with this condition may also experience psychological effects, such as feeling self-conscious or being stared at by strangers.
For most people with Heterochromia Iridis, the condition is nothing more than a unique feature that allows them to stand out from the crowd. There are many famous figures throughout history who have embraced their rare eye condition and made it part of their identity, including David Bowie and Dan Aykroyd. So, if you or someone you know is living with Heterochromia Iridis, take comfort in the fact that this rare condition can be a source of beauty and uniqueness.
Stargardt Disease – A Genetic Disorder That Can Lead to Blindness

Stargardt Disease is a rare eye disorder that affects the macula, a small spot near the center of the retina responsible for detailed central vision. It is caused by an inherited genetic mutation that disrupts retinal functioning, leading to progressive vision loss and eventually total blindness. Symptoms may include difficulty reading or recognizing faces, decreased central vision, and distorted vision.
Though there is no cure for Stargardt Disease, therapies like low-vision aid can help to manage the symptoms and make everyday life more manageable. Photodynamic therapy (PDT) has also been used to treat the disease in some cases. In PDT, a drug called verteporfin is injected into the bloodstream, and then activated by a laser. This helps to prevent further damage to the macula, slowing down the progression of the disease.
Living with Stargardt Disease can be difficult, but with proper treatment and support from family and friends, it is possible to lead an active life despite vision loss. It’s important to stay connected with the rare eye disease community, and to seek out resources that can provide support and information. With the right help, people living with Stargardt Disease can still lead rewarding lives.
If you or someone you know has been diagnosed with a rare eye disorder like Stargardt Disease, it’s important to consult with a specialist and familiarize yourself with the disorder. With the right care, it’s possible to manage symptoms and live a full life despite vision impairment.
Uveal Effusion Syndrome – An Autoimmune Disorder That Impacts the Retina
Uveal Effusion Syndrome (UES) is an extremely rare eye disease characterized by the accumulation of fluid in the back of the eyeball. It is an autoimmune disorder, meaning that instead of fighting off foreign invaders, our own immune system attacks healthy tissue in the eyes. In UES, white blood cells gather around the uveal tissue, leading to inflammation and fluid buildup.
Unfortunately, UES has no known cure and is thought to be idiopathic in nature. Symptoms can include blurry vision, floaters, light sensitivity, pain, redness and swelling of the eye. If left untreated it can lead to glaucoma or even blindness. Treatment typically includes corticosteroid injections or anti-inflammatory medications to reduce the inflammation.
UES can be a difficult condition to live with, but with proper management and care, those who suffer from UES can still live full and healthy lives.
Albinism – A Genetic Condition That Causes Pigment Loss in the Eyes

Albinism is a rare genetic condition that causes the partial or complete absence of pigment in a person’s eyes, skin, and hair. It occurs in all racial and ethnic groups. Albinism is an inherited condition caused by a recessive gene passed down from both parents to their children. Individuals with albinism typically have lighter hair, skin, and iris color than those without the condition.
They may also have vision problems such as near or farsightedness, photophobia (sensitivity to light), and nystagmus (involuntary eye movements). In some cases, albinism can lead to ocular disorders that affect a person’s ability to see. These disorders can range from reduced visual acuity to complete blindness.
Albinism is a rare eye disease in humans, with only about one in every 20,000 people worldwide having it. In the United States, one in 17,000 people are born with albinism. While there is no cure for albinism, individuals living with the condition can take steps to protect their eyes from the sun and other environmental factors by wearing sunglasses and hats with wide brims.
Additionally, following up with regular eye examinations is important for individuals living with albinism as early detection of any ocular disorders is key to preventing vision loss.
If you or a loved one has been diagnosed with albinism, it is important to be aware of the potential risks and treatments available. There are supportive communities online and in-person that can help individuals living with albinism adjust to life with the condition. With proper care, those living with albinism can manage their condition and live a happy, healthy life.
Leber Congenital Amaurosis (LCA) – Another Genetic Eye Disease that Causes Blindness
Leber Congenital Amaurosis (LCA) is a rare eye disease that causes severe vision loss in humans. It is the most common form of inherited retinal dystrophy and usually appears early in life. LCA is caused by a genetic defect, which means it can be passed down from parent to child. Symptoms may include extreme light sensitivity, poor night vision and an inability to detect colors.
In some cases, LCA can lead to complete blindness. Treatment options are limited but include surgical procedures, gene therapy and stem cell treatments. With early diagnosis and treatment, it is possible to slow the progression of the disease or even restore some level of vision.
Unfortunately, there is no cure for Leber Congenital Amaurosis, so it is important to research the condition and know the signs in order to detect it as early as possible.
If you or someone you know has been diagnosed with Leber Congenital Amaurosis, there are resources available to help. Organizations such as the Foundation Fighting Blindness provide support and information on treatment options for rare eye diseases. It’s also important to find an experienced ophthalmologist who can help manage the condition and provide advice on lifestyle modifications that may reduce its impact. With support and understanding, individuals with LCA can continue to live full, productive lives.
Optic Nerve Hypoplasia – A Rare Genetic Disease That Affects Vision Development
Optic Nerve Hypoplasia (ONH) is a rare eye condition that affects the development of the optic nerve and can lead to vision loss in humans. It is caused by a genetic mutation in which there is a deficiency of nerve fibers in the optic nerve, resulting in poor development and impaired functioning. ONH is usually diagnosed at birth, but can be detected later in life as well.
When there is a deficiency of nerve fibers in the optic nerve, it affects the development of vision and other parts of the eye. This can lead to a range of vision problems including strabismus (crossed eyes), amblyopia (lazy eye), or even blindness. It can also lead to a range of other problems such as abnormal pupillary responses, nystagmus (involuntary eye movements), and double vision.
Although there is no known cure for Optic Nerve Hypoplasia, treatment options are available. Treatment focuses on providing supportive care to minimize the effects of vision loss, improving the quality of life, and preventing further damage. Treatment may include vision therapy, surgery, glasses or contact lenses, medications, and lifestyle modifications.
Living with ONH can be challenging but with proper care and support it is possible to lead a full and rewarding life. It’s important to remember that even though rare eye diseases like Optic Nerve Hypoplasia can be difficult, there are still many resources available to help. Seeking out the right support and advice is key for living a full and enriching life with ONH.
No matter what stage of life you’re in, it’s important to stay informed and up-to-date on the latest treatments and research for rare eye diseases in humans. Although a rare eye disease can be difficult to live with, it’s important to remember that you are not alone and there is always hope and help available.
Keratoconus – A Progressive Corneal Degeneration Disease
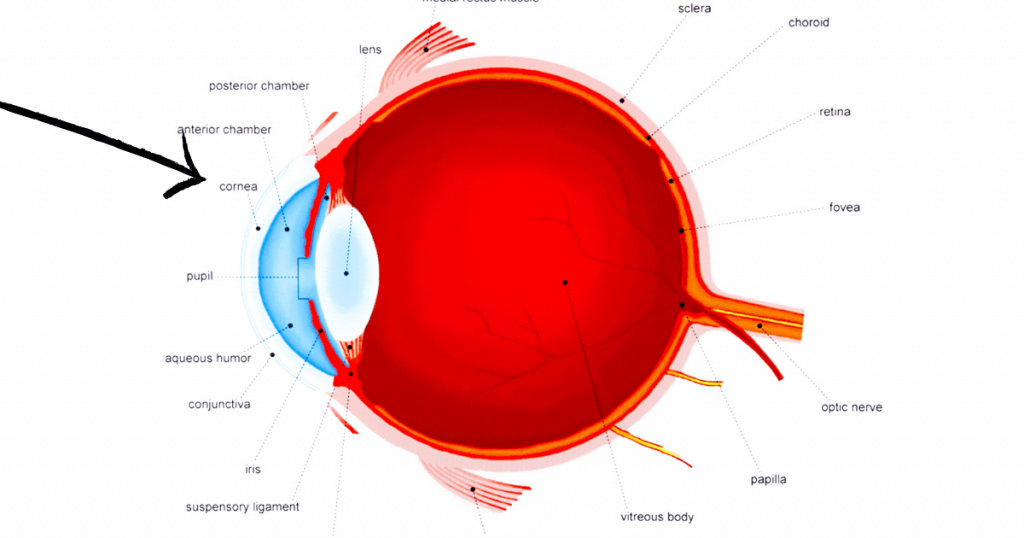
Keratoconus is a rare eye condition that affects the cornea, or the clear outer layer of the eye. It causes the normally round shape of the cornea to become thin and cone-shaped, which can cause distorted vision and increased sensitivity to glare. It is considered a progressive condition, meaning it tends to get worse over time, and there is no cure for it. Symptoms may include blurred or hazy vision, frequent eye strain, light sensitivity, double vision in one eye, and contact lens intolerance.
There are a variety of treatments available to help manage the symptoms of keratoconus including glasses, soft contact lenses, hard contact lenses, corneal cross-linking, and corneal implants. It is important to consult with an eye doctor regularly to help manage the condition and prevent further vision loss. In some cases, surgery may be recommended to provide a more permanent solution.
Coloboma – Congenital Defect Affecting The Structure Of The Eye
Coloboma is a rare eye condition that affects the structure of the eye. It is caused by a congenital defect that results in a hole or gap in the tissue of the eye, usually at the level of the iris, retina, or optic nerve. It can be present at birth, or can occur during childhood development. Symptoms may include abnormal vision, light sensitivity, and eye redness.
There is no cure for coloboma, but treatment options are available to help manage symptoms and reduce the risk of further vision loss. Treatment may include glasses or contact lenses, medications to reduce inflammation or prevent infection, corrective surgery, laser treatments, and lifestyle modifications. In cases where vision cannot be improved, other methods may be used to help improve the quality of life.
It is important to seek medical attention right away if you or your child has signs and symptoms of coloboma. Early detection is key in order to get the proper treatment and prevent further vision loss. Consulting with an eye doctor regularly can help ensure that any necessary treatments are put into place as soon as possible.
Coloboma can be a difficult condition to live with, but there are still many resources available to help you or your child live full and enriching lives. Seeking out the right support and advice is key in managing the effects of coloboma and living life to the fullest.
No matter what stage of life you’re in, it’s important to stay informed and up-to-date on the latest treatments and research for rare eye diseases. By taking these steps, you can make sure that you are doing whatever is necessary to protect your vision and live a fulfilling life.
Fuchs’ Dystrophy – A Serious Corneal Problem that can Cause Vision Loss
Fuchs’ Dystrophy is a rare eye disease that affects the corneal layer of the eyes and can lead to vision loss if left untreated. It is caused by the deterioration of cells in the cornea resulting in swelling, making it difficult for them to stay clear which leads to blurry vision. The disease most commonly affects people in their 50s and 60s, although it can affect people of any age.
Symptoms include hazy vision, sensitivity to light, eye irritation and excessive tearing. If left untreated, Fuchs’ Dystrophy can cause severe vision loss due to the swelling of the cornea blocking light from reaching the retina.
Treatment for Fuchs’ Dystrophy typically involves replacing the affected cells with healthy ones. This can be done through a corneal transplant, which is a surgical procedure that replaces all or part of the cornea. There are also medications and eye drops available to help reduce symptoms and slow down deterioration.
Fuchs’ Dystrophy may be rare, but keeping an eye on your vision is important in preventing the condition from worsening. If you experience any of the symptoms listed above, be sure to visit your optometrist or ophthalmologist for a comprehensive eye exam. Early diagnosis and treatment can help prevent vision loss and keep your eyes healthy.
Retinoblastoma – A Sinister Form Of Cancer Originating In the Back Portion of the Eye
Retinoblastoma is a rare form of cancer originating in the back portion of the eye, which is known as the retina. It is one of the most common forms of eye cancer among children and can be life-threatening if not detected and treated early on with the average age at diagnosis being three years old. This type of cancer typically develops from mutations in a gene called retinoblastoma, which is responsible for controlling the growth of normal cells in the retina.
When left untreated, Retinoblastoma can spread to other parts of the body and become deadly. Symptoms include a white glow in one or both eyes, redness or swelling of the eye, a decrease in vision, and occasionally pain. If caught early enough, Retinoblastoma can be treated with surgery, radiation therapy, chemotherapy, or a combination of treatments.
Retinoblastoma is one of several rare eye diseases in humans that can be detected early on if parents or caregivers are aware of the signs and symptoms. Regular eye exams and scans can help detect any abnormalities of the eye that could be indicative of Retinoblastoma or other rare eye diseases in humans. The earlier these conditions are detected, the more likely successful treatment can be obtained.
As with all forms of cancer, it is important to monitor your child’s health closely, be aware of any changes to their eyes or vision, and seek medical attention as soon as possible. Early detection of Retinoblastoma can save your child’s life. With proper treatment, most children with this rare eye disease can go on living long and healthy lives.
Take care of your eyes and the eyes of those you love! A little extra precaution can go a long way in protecting against rare eye diseases in humans.
Neuromyelitis Optica (Devic Disease) – An Unpredictable Autoimmune Disease
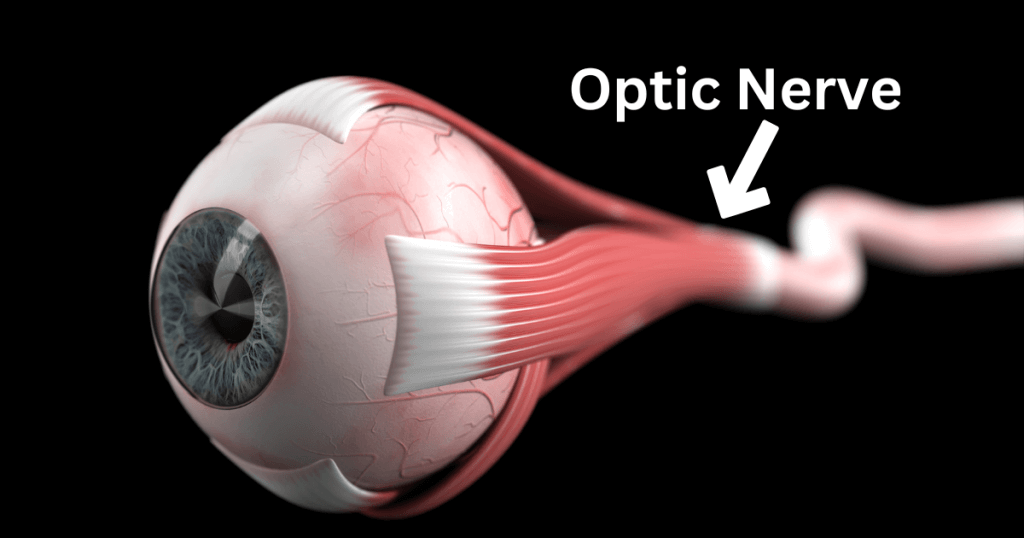
Neuromyelitis Optica (NMO) or Devic Disease is a rare and unpredictable condition that affects the optic nerve and spinal cord of the central nervous system. It is an autoimmune disorder, meaning it occurs when the body’s own immune system mistakenly attacks healthy tissues. NMO can cause inflammation, swelling, and damage to the brain and spinal cord, leading to vision loss and neurological problems.
Symptoms of NMO include blurred or cloudy vision, double vision, eye pain, light sensitivity, and difficulty with balance. Other symptoms may include seizures or muscle weakness. NMO is often misdiagnosed as multiple sclerosis (MS) due to their similar appearance on MRI scans. However, NMO usually affects only the eyes and spinal cord while MS has a more widespread central nervous system involvement.
Diagnosis of NMO is made through blood tests and MRI scans. Treatment includes immunosuppressive drugs to reduce inflammation, corticosteroids to reduce swelling, and other medications to control symptoms. In some cases, surgery may be needed to repair or replace damaged tissue.
NMO is a rare and unpredictable condition, but if diagnosed early, patients can receive treatment and live relatively normal lives. It’s important for those who experience any of the symptoms associated with NMO to talk to their doctor about it as soon as possible for proper diagnosis and treatment. Doing so can help limit the progression of this rare eye disease and improve quality of life for those affected by it.
Early Detection and Prevention for Rare Eye Diseases in Humans
Early detection and prevention of rare eye diseases in humans is essential for protecting vision and maintaining ocular health. Unfortunately, many of these conditions are not common and may go undetected until they have caused permanent visual damage. To address this issue, it is important to be aware of the signs and symptoms of rare eye diseases as well as the preventive measures that can be taken.
The most common rare eye diseases in humans include retinitis pigmentosa, Stargardt disease, Usher syndrome, and Leber’s congenital amaurosis. These conditions can cause progressive vision loss due to the death of photoreceptors in the retina. Early detection is important because it allows for the implementation of treatments that can slow down the progression of the disease.
Prevention is also key to avoiding vision problems associated with rare eye diseases. The most effective way to prevent these conditions is through regular comprehensive eye exams and preventive genetic testing. Comprehensive eye exams allow for early detection and treatment, while preventive genetic testing can alert patients to their risk of developing rare eye disease.
It is important to remember that many rare eye diseases in humans are progressive, meaning they will continue to worsen over time regardless of treatment. Therefore, it is essential to seek medical advice and follow-up care from an ophthalmologist for those who are at risk for these conditions. Early diagnosis and preventive measures can help to protect and preserve vision for those with rare eye disease.
If you or someone you know is experiencing any changes in vision, it’s important to talk to an ophthalmologist. Early detection and prevention are key to avoiding permanent damage from rare eye diseases. Stay informed, observe changes in your vision, and take the necessary steps to protect your eyes.
You may not know it, but you could be at risk for one of these eleven rare eye diseases.
These eleven rare eye diseases can sneak up on you without warning and cause severe vision loss if left untreated.
Early detection is key to getting the proper treatment for these eye diseases. But that’s not all – there are also preventative measures that you can take to protect yourself from developing one of these rare eye diseases in humans.
Now let’s take a look at some questions and answers you may have about rare eye diseases in humans.
FAQ’s for Rare Eye Diseases in Humans
Is heterochromia harmful?
Heterochromia is a condition where the eyes are two different colors, typically a combination of blue and brown, or green and brown. In most cases this condition is harmless, as it has no impact on vision or any other part of the body. However, in rarer cases heterochromia can be caused by an underlying medical issue like Horner Syndrome or Waardenburg Syndrome.
What famous people have heterochromia?
The condition of heterochromia, or having two different colored eyes, is quite rare but can be found in a few famous people. Actors and musicians such as Kate Bosworth, Mila Kunis, Christopher Walken, and Kiefer Sutherland have this condition.
You can see the other notable people with heterochromia right here.
What are the 3 types of heterochromia?
Partial Heterochromia – In this type of heterchromia, an individual has two different colors in one eye but within one iris. This color variation may present as a ring of color around the pupil or an irregularly shaped patch on the iris that is much darker than the surrounding tissue.
Sectoral Heterochromia – Sectoral heterchromia occurs when somebody has two distinct sections – with each section showing a different colored pattern within one iris. It usually looks like someone who has drawn a line horizontally or vertically through their eye!
Central Heterochromia – Central heterchromjai occurs only if there are three colors visible in one eye: One large color surrounded by either lighter or darker rings around it’s outside edge near to the pupil. The colors can range from green to blue to brown and even violet!
When does Stargardt’s disease start?
Stargardt’s disease is a rare genetic condition that causes progressive vision loss in childhood and adolescence. It usually begins between the ages of 6 and 20, although it can start as early as infancy or later on in life.
Do people with Stargardt’s go completely blind?
No, not necessarily. Stargardt’s is a genetic disorder that causes progressive vision loss or blindness in children and young adults. It affects the macula, which is the tiny central area of the retina. While up to 10% of cases are associated with total blindness by 20 years of age, many people with Stargardt’s retain some degree of usable vision throughout their lives.
Is Stargardt’s a disability?
Yes, Stargardt’s Disease is a disability and can have significant effects on a person’s life. It is an inherited disorder of the retina that can cause vision loss in one or both eyes. Symptoms often begin in early childhood and gradually worsen over time, leading to blurred central vision and reduced color vision, as well as decreased night-vision capabilities.
What are the three components of uveal tract?
The uveal tract is composed of three main components: the iris, ciliary body, and choroid.
The iris is a thin, colored muscular diaphragm in front of the lens that controls how much light enters into the eye. It also determines eye color because it comes in various colors such as blue, green or brown.
The ciliary body is a muscular structure that surrounds the lens and produces aqueous humor which is important for intraocular pressure control and nutrition to ocular structures like the crystalline lens.
Finally, the choroid sclera layer contains capillaries and melanocytes which provide nourishment to outer retinal layers while absorbing scattered light to allow better vision.
Together these three components work together as an integral part of maintaining healthy vision. They are responsible for controlling light entering into our eyes by regulating pupil size via contraction or expansion of its muscles within the iris and regulating fluid balance inside our eyes through production of aqueous humor from ciliary processes.
By providing nourishment to outer retinal layers with its blood vessels within Choroid Sclera layer they make sure our retina stays healthy throughout our lives allowing us to see clearly all around us!
How does albinism affect eyes?
Individuals with albinism usually have very light skin as well as white or almost colorless hair. In terms of eyesight, albinism can cause vision issues due to a lack of pigment in the ocular structures such as the iris and retina. This lack of pigment causes problems like reduced visual acuity, photophobia (sensitivity to light), strabismus (cross-eyed) and amblyopia (lazy eye). Optic nerve hypoplasia is also common which causes poor depth perception, decreased visual fields and nystagmus (involuntary eye movements).
Can you drive with ocular albinism?
It depends. While people with ocular albinism can obtain driver’s licenses in some states, it is important to note that ocular albinism is a complex condition that affects eyesight significantly. Depending on the severity of the condition and its associated vision issues, driving may be dangerous or impossible even if a person has obtained a license.
Can females have ocular albinism?
Yes, females can have ocular albinism.
Women with ocular albinism experience different vision problems because of their lack of pigment in their iris and retina. They often have reduced visual acuity (clarity) in one or both eyes and difficulties with depth perception, light sensitivity, astigmatism (blurry vision), tracking abilities (following movements), glare issues, nystagmus (uncontrollable eye movement), decreased reading fluency and night blindness.
What are the 4 stages of a Leber Congenital Amaurosis (LCA)?
There are four stages of Leber Congenital Amaurosis, each with its own unique set of symptoms:
Stage 1: At this stage, babies are born with near-normal vision or only slight visual defects such as blurriness and sensitivity to bright lights. As they grow up, their symptoms gradually worsen over time but may not be noticeable until adulthood due to compensation.
Stage 2: Symptoms become more severe at this point, with individuals experiencing gradual central field loss (tunnel vision), photophobia (light sensitivity), nystagmus (rapid uncontrolled side-to-side movements), color deficiency and strabismus (crossed eyes).
Stage 3: Visual acuity drops significantly during this stage as affected individuals experience night blindness and blind spots while stationary objects start appearing blurry even when looking straight ahead.
Stage 4: Affected individuals begin losing peripheral vision at this stage resulting in total legal blindness by age 20. They also develop progressive myopia which causes further deterioration of vision quality and depth perception difficulties such as trouble judging distances accurately. In addition, retinal arteries start narrowing leading to retinopathy that slowly continues throughout life eventually causing complete blindness.
In conclusion, Leber Congenital Amaurosis is a serious condition that affects the retina’s ability to process light normally leading varying levels of visual impairment from mild blurring up to complete legal blindness depending on the severity of the condition; however it can be managed through early diagnosis so people impacted by LCA can still live full lives!
How is LCA diagnosed?
The diagnosis of Leber Congenital Amaurosis requires an extensive medical evaluation by an ophthalmologist who specializes in diseases of the eye. During the examination, they will usually perform various tests including visual acuity assessments, fundus photography and fluorescein angiography as well as specialized imaging tests such as optical coherence tomography and electrophysiology studies. Genetic testing may also be done if there appears to be an inherited basis for the disorder.
Once the appropriate diagnostic procedures are completed, it’s possible for doctors to accurately diagnose LCA with very high accuracy rates – although sometimes additional tests or evaluations may be necessary before making a definitive conclusion about whether or not someone has LCA.
Some cases may require confirmation through genetic testing at specialty labs which specialize in diagnosing complex disorders caused by gene mutations or deletions; however even without these tests it’s still possible for doctors to make a diagnosis based on symptoms and clinical findings present during examination.
What makes Luxturna suitable treatment for LCA?
Luxturna has been approved by the FDA as a suitable treatment for Leber Congenital Amaurosis (LCA) due to its ability to effectively reverse vision loss and improve visual function in patients who suffer from this rare genetic disorder. LCA is caused by mutations in the RPE65 gene, which results in impaired development of photoreceptor cells in the retina.
Luxturna works by delivering a corrective copy of that gene directly into cells via an injectable viral vector, allowing them to produce functional proteins that lead to improved retinal structure and vision.
Studies have found that when treated with Luxturna, most patients experience improved vision within one month and maintain it over time. It has been seen to improve visual function even up to three years after injection, which is why it stands out compared other treatments offered for this condition. In addition, it’s also proven effective across a wide range of ages: from young children all the way up to adults over 70 – something few other treatments can offer for LCA.
Is optic nerve hypoplasia life threatening?
In most cases, ONH itself is not life-threatening; however it can have serious implications on an individual’s vision and quality of life.
The severity of ONH depends on how much of the optic nerve is affected and any additional medical conditions that may be associated with it. Generally speaking, children affected with ONH may experience some degree of visual impairment ranging from mild to severe depending on the extent of damage done to the optic nerves. The various levels of vision issues include: reduced sharpness/clarity (visual acuity), degraded peripheral vision (field cuts), color discrimination problems, depth perception issues, and more.
What does a person with optic nerve hypoplasia see?
Generally speaking, people with ONH experience decreased vision or even legal blindness. Depending on how severely their optic nerves have been affected, some may retain very limited light perception and colors can be distinguished by bright light shining directly on it.
For people with ONH that are legally blind or almost completely sightless, they typically lack any type of useful vision in either or both eyes. This means that there won’t be any visual images created; only shapes and shadows can be made out depending on the intensity of existing lights around them.
Does optic nerve hypoplasia get worse over time?
The condition can vary in severity; some may experience mild symptoms while those with more severe cases may be affected by vision loss or even blindness. Unfortunately, ONH does progress over time and its effects can worsen as you get older.
How serious is keratoconus?
If left undiagnosed or untreated it can lead to drastic vision losses, including full blindness.
Since this is an eye disease that progressively worsens over time, early detection is key in order to slow its progression. Oftentimes it can be identified by examining previous medical records or through routine vision tests but many times diagnosing keratoconus often requires advanced imaging techniques such as optical coherent tomography (OCT).
Keratoconus typically affects both eyes but when one eye usually progresses further than the other resulting in a significant difference between them. This difference can manifest itself with visual problems that are difficult to describe as it varies greatly depending on how severe the patient’s case is.
How does a person with keratoconus see?
People with keratoconus can experience symptoms such as glare and halos around lights, inability to focus on near objects, eye strain, poor night vision, frequent changes in eyeglass prescription, unusual sensitivity to light and difficulty driving at night.
Due to the irregular shape of the cornea caused by keratoconus, vision can be blurry or foggy.
Can keratoconus stop naturally?
Unfortunately, it cannot stop naturally; instead, it usually progresses over time.
However, there are a number of treatments for keratoconus that can slow or even halt its progression. These include corneal collagen cross-linking (CXL), Intacs inserts, orthokeratology (crash lens therapy) and phototherapeutic keratectomy (PTK). CXL involves using ultraviolet light to activate riboflavin drops on the cornea which causes small chemical bonds or “links” between collagen fibers in the deep layers of the cornea. This prevents further damage from occurring and may even help restore some lost corneal shape.
What does a person with coloboma see?
As there are many factors involved depending on what exact part(s) are impacted by a person’s coloboma, it’s difficult to provide one definitive answer on what someone sees when living this condition day-to-day. However, general consensus among specialists indicates that people who have been diagnosed likely see objects only partially. Missing vital details such as near peripheral awareness or full view images.
Leading some individuals down particular career paths versus others due solely to limitedly functioning visual capabilities. Taking into consideration when searching for employment opportunities as well as leisure activities involving sight recognition/reading instructions etc.
Ultimately it really comes down to a case-by-case per individual depending on how much location area was invaded by this congenital disorder. Compromising optimum functionality when performing things we typically take for granted requiring little effort seeing-wise.
Is a coloboma a disability?
Yes, coloboma is considered a permanent disability. Coloboma is an ocular disorder caused by an incomplete closure of the choroid fissure during fetal development which results in a defect in one or more parts of the eye, such as the iris, retina, choroid and/or optic nerve. This can lead to partial vision impairment or blindness, depending on how much of the eye is affected.
Does coloboma affect the brain?
Absolutely! Coloboma is an eye disorder that occurs when the structures of the eye fail to develop normally during fetal growth. Generally, colobomas occur in structures such as the iris, choroid, retina and optic nerve; however, they can also include other parts of the eye.
Although most colobomas have no effect on vision or brain function, some cases may be caused by mutations in genes that are crucial for brain development. These mutations can result in neurological conditions such as intellectual disabilities and growth abnormalities which range from being mild to life-threatening.
Do glasses help Fuchs dystrophy?
Glasses can definitely help with Fuchs dystrophy. To treat Fuchs dystrophy, eyeglasses are often used as a corrective solution to improve vision clarity so you can go about your day without feeling hindered by your condition.
How do you slow down Fuchs dystrophy?
Fortunately, there are ways to slow down the progress of Fuchs dystrophy and potentially prevent further vision loss.
The most important step in slowing Fuchs dystrophy progression is to wear sunglasses with UV protection whenever you’re outdoors. This helps protect your eyes from harmful rays which can worsen symptoms like blurred vision, glare, double images and light sensitivity.
Additionally, maintaining good hydration levels is important for protecting against corneal swelling as dehydration raises osmotic pressure in the body which causes cells within the cornea to swell up, which is a symptom of Fuch’s dystrophy. It’s best to aim for 6-8 glasses of water (or more depending on how much physical activity you do) each day in order to stay properly hydrated!
In addition to lifestyle changes like wearing sunglasses and hydrating properly, there are various treatments available that can help slow down the progression of Fuchs’ Dystrophy such as medications like topical steroids or nonsteroidal anti-inflammatory drugs (NSAIDs). Laser surgery techniques such as PTK may also be used in some cases where damaged tissue needs removal from the surface of the eye or when scarring has taken place due to long-term contact lens use.
Finally, it’s important for those living with Fuch’s Dystrophy not to overdo contact lens wear as this could cause problems too so always make sure you follow your doctor’s instructions regarding contact lenses specifically meant for individuals with this condition.
By taking preventive measures such as wearing sunglasses with UV protection and staying adequately hydrated along with continuing treatment plans prescribed by doctors specializing in eye care conditions such as Fuchs’ Dystrophy – it should be possible slow down its progression while preserving existing eyesight over time!
What is the newest treatment for Fuchs dystrophy?
Treatment for Fuchs dystrophy has advanced greatly over the years with new and promising treatments becoming available more frequently.
The newest treatment option currently recommended by ophthalmologists is known as Descemet’s Stripping Automated Endothelial Keratoplasty (DSAEK). This procedure involves removing a thin layer of diseased tissue from your cornea and replacing it with healthy donor tissue that helps restore visual acuity. DSAEK has become so successful due to its non-invasive nature and quick recovery time, allowing most people who undergo this procedure to resume normal activities within 2 weeks.
Another newer treatment for Fuchs dystrophy is Corneal Endothelium Transplantation (CET). Although this type of procedure typically involves an incision, it can provide long-term relief from blurry vision caused by Fuch’s dystrophy.
CET offers an advantage over DSAEK in that it can be tailored specifically for each patient’s eye condition or degree of damage, giving them greater visual acuity than possible previously through standard treatments like LASIK surgery or contact lenses.
No matter which type of treatment you choose, consulting with an experienced ophthalmologist should be a top priority when deciding on which course of action to take regarding Fuchs Dystrophy management. Your doctor will be able to discuss all available options and help you find the one that best suits your needs and lifestyle!
What is the life expectancy of someone with retinoblastoma?
The life expectancy of someone with retinoblastoma is highly variable and depends on the individual case. When caught early, treatment can be incredibly successful and individuals affected by the cancer may have an outcome that is not drastically different than those who are unaffected.
The American Cancer Society estimates that average overall survival rates for retinoblastoma range from 75% to 90%. It’s important to note, however, that the chance of long-term survival will vary greatly depending on where in the eye or orbit this tumor occurs as well as how far it has spread.
What happens to the eye in retinoblastoma?
Retinoblastoma is an aggressive form of eye cancer that affects children and young adults. It occurs when the cells in or around the retina start to grow abnormally, forming a tumor inside the eye.
The most common symptom of retinoblastoma is a white reflection (called leukocoria) from the pupil. This may be noticed in photos taken at night or in low light conditions, as well as when shining light directly into your child’s eyes. Other signs and symptoms can include redness, swelling and/or vision loss in one or both eyes.
Does retinoblastoma cause death?
Yes, retinoblastoma can cause death. This form of cancer affects the eyes and is most commonly diagnosed in children ages 5 and under. When caught early, it can be treated with a combination of surgery, chemotherapy, radiation, and targeted treatments such as cryotherapy or thermotherapy.
However, if retinoblastoma spreads beyond the eye area to other parts of the body such as the brain or spine – known as metastatic disease – this poses greater risks for life-threatening side effects from treatment.
How serious is neuromyelitis optica?
Neuromyelitis optica (NMO) is a serious and potentially life-threatening autoimmune disorder that affects the central nervous system. It is characterized by inflammation of the optic nerves, which can cause vision loss, as well as by inflammation of the spinal cord and brainstem, resulting in weakness or paralysis in various parts of the body.
Although NMO is rare, it can have wide-ranging effects on those who suffer from it.
Is Devic’s disease worse than MS?
Neuromyelitis Optica (Devic Disease) is considered by some to be worse than multiple sclerosis (MS). While the symptoms of Devic Disease can often mimic those of MS, this autoimmune disorder directly affects the optic nerve and spinal cord with inflammation. As a result, it can cause vision loss and paralysis in addition to other neurological issues that may not be found in MS patients.
The damage caused by Devic Disease tends to occur quickly, over a matter of weeks or months, while damage from MS can take years or decades to manifest. Because the destruction often takes place rapidly with Devic Disease, there’s less time for doctors to intervene before significant impairment has occurred. This makes it much more difficult for them to treat and manage its effects on the patient’s well-being.
How long can you live with neuromyelitis optica?
Living with neuromyelitis optica (NMO) is a highly individualized experience and there is no single answer that fits everyone. Generally, NMO can be a chronic or acute illness depending on the person, as well as how they handle their treatment and lifestyle.
The good news is that many people diagnosed with NMO are able to lead active and productive lives. However, some individuals may experience relapses which may require more intense therapies or medications to manage the condition effectively.
Final Thoughts
We hope this article has helped you to understand some of the rare eye diseases in humans, their causes, symptoms and treatments. Early detection is key for getting proper treatment and it’s important to take preventive measures such as regular comprehensive eye exams and genetic testing.
Remember that many rare eye diseases in humans are progressive so seeking medical advice from an ophthalmologist is essential if you or someone you know experiences any changes in vision. By staying informed on these eleven rare eye conditions, observing changes in your own vision, and taking necessary steps to protect yourself – we can all work together towards preserving our sight!
Thank you for reading and have an amazing day!















